Services
Physician Peer Review
Board-certified specialists answer specific questions related to utilization of care and claimant treatment plans, compensability and extent of injury issues through comprehensive medical evidence-based assessments of claimant medical records.
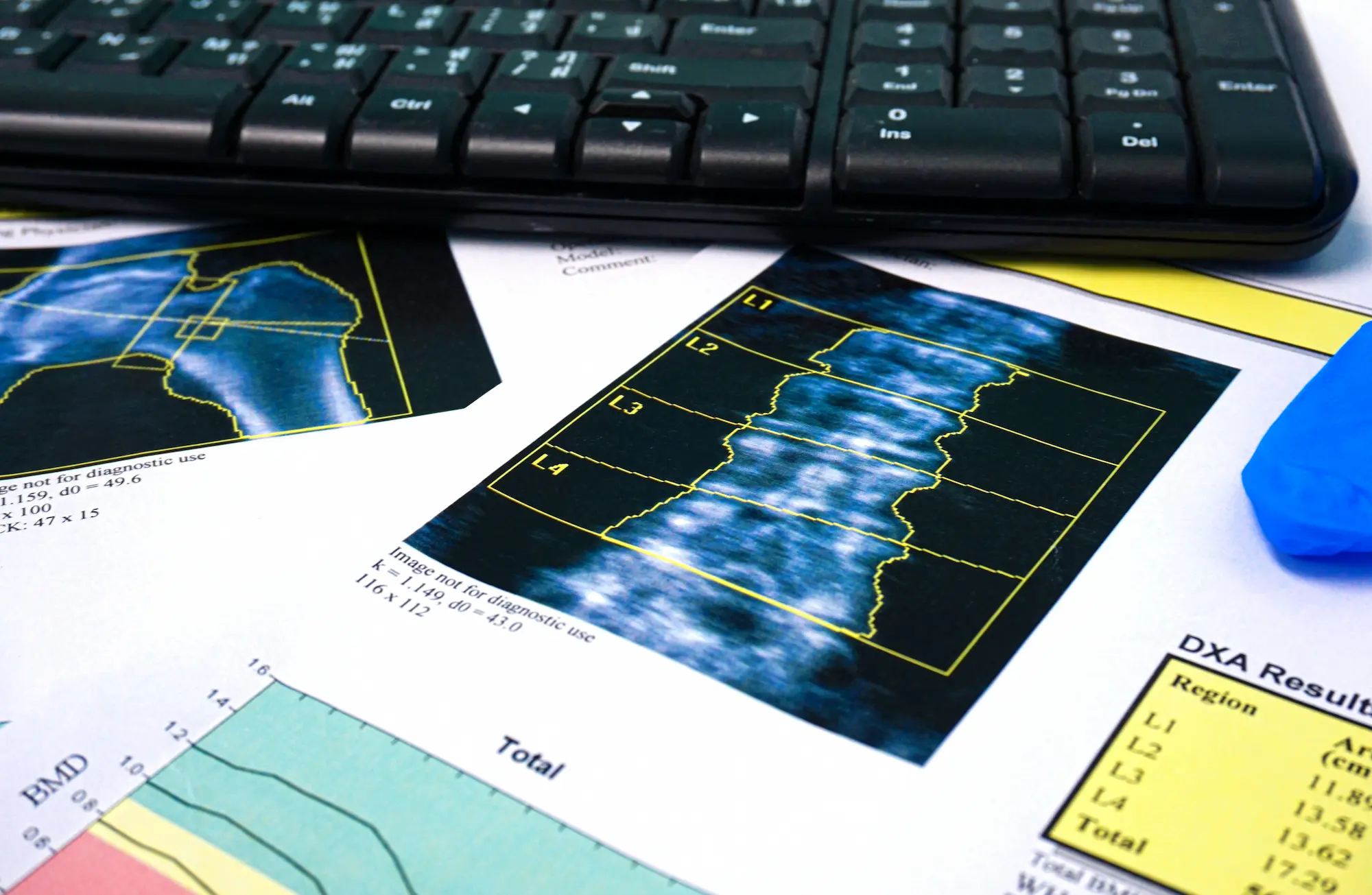
Impairment Rating Review
Impairment rating reviews ensure that your claimant’s impairment rating meets the standard of the specific guidelines insured specific to the applicable jurisdiction, the statute, and appeals panel decisions.

Baseline clinical assessment
C3′s licensed and board certified physicians thoughtfully assess mechanisms of injury and provide you with an early evaluation of what is and what does not appear to be compensable.
DWC 32 Processing with Summary
C3’s professional staff completes the DWC-32 and submits the completed form to the adjuster for approval prior to submitting to DWC. We sort and summarize the medical records with special attention and detail related to the questions posed to the Designated Doctor. We ensure records and summary are provided to the Designated Doctor in compliance with DWC rules and regulations. Following the date of the exam, our staff will contact the DD’s office, confirm attendance and provide the adjuster with status updates during the process. If the adjuster submits the 32 form, we can still complete a Claims File Analysis and handle the claim as previously discussed.


Cumulative Impact
An analysis of the current impairment rating with an assessment of a previous compensable injury’s Impairment Rating as it relates to seeking contribution.
Claims File Analysis
A CFA report provides a comprehensive medical record review, listing all disputes (per PLN-11), a full medical timeline, return to work history (per DWC 73), previous DDE’s and RME’s. Records are organized for the designated doctor and outlined in an efficient summary.


Diagnostic Re-Read
Let us Customize a Plan for You!
For a customized workers compensation management plan, built around your specific goals and needs, please contact us today.
